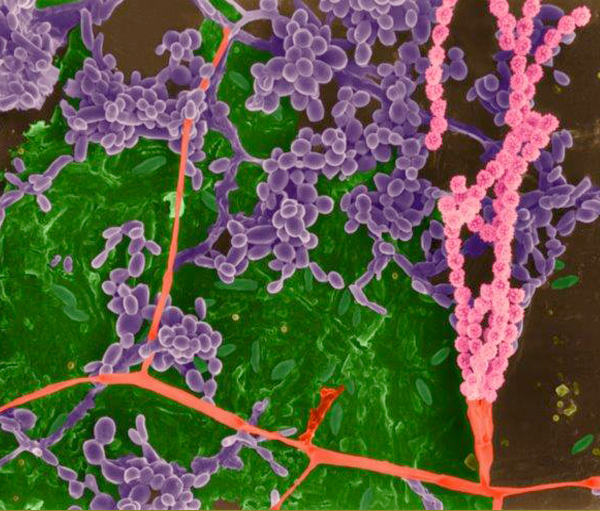
© Dennis Kunkel Microscopy
Home Resources Pathogens Expert Consulting: What is Vibrio vulnificus?
Expert Consulting: What is Vibrio vulnificus?

© Dennis Kunkel Microscopy
Vibrio vulnificus is a gram negative bacterium, that is biochemically similar to Vibrio parahaemolyticus and is most often associated with food borne illness after eating raw or inadequately cooked seafood, especially raw oysters.
What diseases are caused by Vibrio vulnificus?
Vibrio vulnificus is mainly implicated in gastrointestinal illness characterized by vomiting, diarrhea and abdominal pain. Vibrio vulnificus can also cause an infection or ulceration of the skin when open wounds are exposed to seawater.
Who is at a higher risk of infection with Vibrio vulnificus?
Infection with Vibrio vulnificus may cause complications such as septicemia in people with chronic liver disease, chronic alcoholism or hemochromatosis and those that are immunocompromised. This disease is of special concern to those with chronic diseases of the liver.
Incubation Period
The incubation period for Vibrio vulnificus is usually between 12 - 72 hours after consuming raw or undercooked seafood.
Epidemiology of Vibrio vulnificus
This disease is not transmitted person to person. Sporadic cases are reported each year. Vibrio vulnificus is a free living organism found in marine waters. This organism is of special concern to the oyster industry and is found routinely in cultured oysters.
This is a very serious disease in that approximately one third of the patients seen for care associated with wound infections are either in shock or develop hypotension within 12 hours of hospitalization. Three quarters of the patients develop bullous skin lesions, thrombocytopenia and often disseminated intravascular coagulation.
Over 50% of the patients with primary septicemia die and the mortality rate exceeds 90% among those who become hypotensive. Vibrio vulnificus can also infect wounds sustained while in contact with coastal or estuarine waters (boating accidents, fisherman oyster shuckers) and can range from mild, self limited lesions to rapidly progressive cellulites and myositis.
Diagnosis
This disease is diagnosed by culturing the organism from wounds, stool, or blood. Confirmation of the organism sometimes requires the use of DNA probes or numerical taxonomy in a reference laboratory.
Treatment
Vibrio vulnificus infection is treated with antibiotics. Doxycycline or a third-generation cephalosporin (e.g., ceftazidime) is appropriate. Tetracycline, chloramphenicol or penicillin could be used as a second line of therapy.
Vibrio vulnificus path chart
View a path chart for Vibrio vulnificus.
Contact EHA Consulting Group today for more information about how we can assist your company.
We offer services for
- Retail Food Safety
- Restaurant Food Safety
- Manufacturers
- Food Trucks
- Drugs & Cosmetics
- Melons & Cantaloupes
- Produce
- Warehouses
- Food Packaging & Packaging Materials