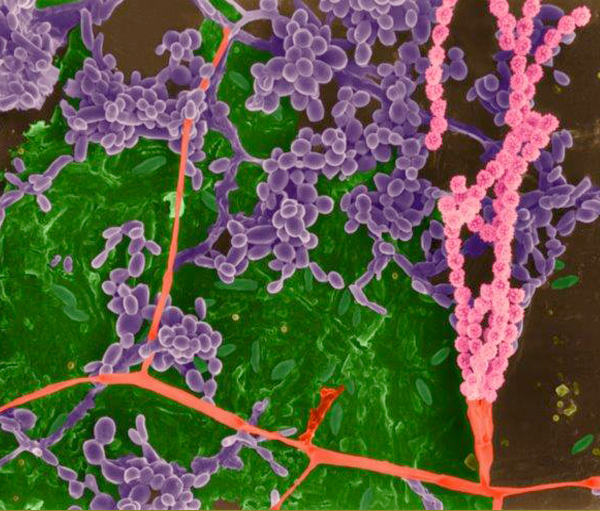
© Dennis Kunkel Microscopy
Home Resources Pathogens What is Clostridium difficile?
What is Clostridium difficile?

© Dennis Kunkel Microscopy
Clostridium difficile is a spore-forming, anaerobic gram-positive bacterium that normally grows in the human gastrointestinal tract.
What diseases are caused by Clostridium difficile?
Clostridium difficile is the major cause of pseudomembranous colitis (inflammation of the colon) and antibiotic-associated diarrhea. Clostridium difficile manifests as a disease- causing organism when other normal intestinal flora are diminished by the use of antibiotics, allowing Clostridium difficile to flourish. The disease is characterized by symptoms of acute, watery foul smelling diarrhea, abdominal cramps, fever and is sometimes associated with blood and mucous in the stool.
Who is more susceptible to infection from Clostridium difficile?
People who are on antibiotics such as ampicillin and clindamycin are specifically susceptible to the disease. The disease is also prevalent in hospitals and nursing homes where, Clostridium difficile and its spores are abundant, and the use of antibiotics is frequent.
Epidemiology of Clostridium difficile
Clostridium difficile is a toxin-forming, spore-producing organism. The preformed toxin is responsible for the watery diarrhea. The transmission of the disease can occur from person to person spread. Clostridium difficile spores survive in the environment for up to 70 days and can be transmitted by direct spread from an infected surface. Strict hand-washing and proper handling of contaminated sites are very important to prevent the spread of disease, especially in health care settings.
Incubation Period
Not precisely known; usually less than 7 days.
Diagnosis
Identification of the clostridia toxin and culture of the organism from infected stool specimen. An endoscopy is helpful in identifying and locating pseudomembranous colitis.
Treatment
Most patients recover upon discontinuing the offending antibiotic, along with supportive measures. The diarrhea usually stops in 1-4 days after discontinuing the antibiotic in healthy individuals. In severe cases a 14-day course of metronidazole or vancomycin is required.
Clostridium difficile path chart
View a path chart for Clostridium difficile.
Contact EHA Consulting Group today for more information about how we can assist your company.
We offer services for
- Retail Food Safety
- Restaurant Food Safety
- Manufacturers
- Food Trucks
- Drugs & Cosmetics
- Melons & Cantaloupes
- Produce
- Warehouses
- Food Packaging & Packaging Materials